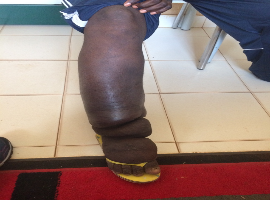
A 25-year-old patient from Guine-Bissau has been referred for edema of the right lower limb for 2 years. He associated the onset of the condition with an interdigital lesion on the ipsilateral foot, with purulent drainage for several weeks, and did not perform dressing care. Since then, he has been treated with multiple cycles of antibiotics, without any effect. Progressive worsening of edema and cutaneous hyperkeratosis was observed instead. Given the epidemiological exposure, clinical manifestations and time of evolution, the diagnosis of elephantiasis due to chronic filariasis was made.
Lymphatic filariasis is the most common cause of lymphedema in endemic countries. It is caused by nematode parasites that invade the lymphatic and subcutaneous tissues. The infection is transmitted by a mosquito bite, which introduces a larva in the third stage of development into the skin. The larvae later mature and, after mating between male and female larvae, release microfilariae into the bloodstream. Adult larvae cause occlusion of lymphatics and damage lymphatic drainage, eventually leading to the development of lymphedema and the skin changes seen in elephantiasis.
The most common acute manifestation of lymphatic filariasis is acute dermatolymphangioadenitis attacks. They are caused by bacterial infections of the skin and are associated with the progression of lymphedema.
The diagnosis is made most of the time by the clinic and epidemiological context. After lymphedema is established, most laboratory tests are negative.
The treatment of choice for lymphatic filariasis is Diethylcarbamazine (DEC) in a single dose, due to its micro and macrofilaricidal effect, preventing the development of chronic complications. However, when lymphedema is established, treatment is only supportive. The treatment of outbreaks of acute dermatolinfangioadenitis involves antibiotics. Its treatment is important, since its occurrence leads to the progression of lymphedema.
Keywords: Lymphatic filariasis; Endemic disease