Case Presentation: A 74-year-old female with medical history significant for hypertension, hyperlipidaemia and hypothyroidism comes with midsternal chest heaviness after a fall the day before. She also had soreness on the left side of her chest that worsens with deep breath or movement. In the emergency department, she was found to be in atrial fibrillation with rapid ventricular response with heart rate of 158 beats per minute and was given diltiazem push and started on a drip. Her blood pressure dropped to 70/43 mm Hg immediately and she had multiple pauses on the telemetry. Diltiazem drip was stopped and she was given intravenous fluid bolus of 1 L normal saline.
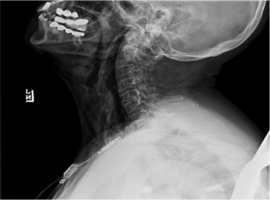
The patient had a 2D-echocardiography (ECHO) which showed ejection fraction of 55-60%, normal ventricular size, wall thickness and systolic function. It was then decided to take her up for a pacemaker insertion. On day 2 of hospitalization, she had a dual chamber pacemaker device (magnetic resonance imaging compatible) inserted via subclavian vein puncture with use of active fixation leads for both atrial and ventricular pacing. The procedure was unremarkable without complications. The next day, the patient complained of chest tightness, neck pain, and facial swelling. Chest x-ray (CXR) was done which only showed a small left apical pneumothorax. Electrocardiogram (EKG) was unremarkable. Subsequent days, since pain and swelling did not subside, CXR and lateral neck radiographs were performed two days later which showed bilateral worsening subcutaneous emphysema with small left-sided pneumothorax as shown in Figure 1.
The patient was monitored over the next few days and subcutaneous emphysema was gradually reduced with conservative treatment confirmed by serial radiographs. Pacemaker interrogation revealed no change in lead data.
Discussion: Pacemaker insertion is associated with complications acute, directly after implantation, early up to 3 months and late beyond 3 months. Acute complications can be pneumothorax, bleeding in the pleural space, hematoma, central vein perforation, electrode dislocation, or inappropriate pacemaker functioning. Long-term complications can be pacemaker pocket infection, or thrombosis of vein with inserted electrodes [1]. The patient presented with a small left pneumothorax complicated by subcutaneous emphysema. The pneumothorax was from the insertion of pacemaker electrodes via subclavian vein and the course can be variable from nearly asymptomatic to acute symptoms such as chest pain, dyspnoea, cyanosis or shock. The management of large pneumothorax involves the insertion of the chest tube and subcutaneous emphysema, in most cases, only requires conservative and symptomatic management.
Keywords: Pacemaker; Subcutaneous emphysema; Complication