Minghsun Liu*
Wound Technology Network, Hollywood, Florida
Prime West / Centinela Hospital Medical Center IM Program, Inglewood, California
California University of Science and Medicine, Colton, California
*Corresponding author: Minghsun Liu, Wound Technology Network, Hollywood, Florida; Prime West / Centinela Hospital Medical Center IM Program, Inglewood, California; California University of Science and Medicine, Colton, California.
E-mail: mliu@alum.mit.edu
Received: March 21, 2024; Accepted: April 04, 2024; Published: April 15, 2024
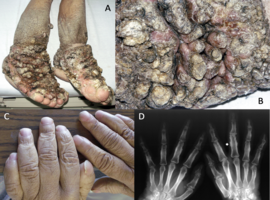
Citation: Minghsun Liu. Thyroid Dermopathy and Acropachy. Clin Image Case Rep J. 2024; 6(4): 392.