Badr Tarif*, Ibn Sbih Oualid, Aymane Jbilou, Younes Aggouri and Said Ait laalim
Department of General Surgery, Mohammed VI University Hospital, Faculty of Medicine and Pharmacy, Abdelmalek Essaadi University, Tanger, Morocco
*Corresponding author: Badr Tarif, Department of General Surgery, University Hospital Center of Tangier, Abdelmalek Essaâdi University of Tangier, Morocco.
E-mail: tarif.badr@gmail.com
Received: July 19, 2025; Accepted: August 02, 2025; Published: August 15, 2025
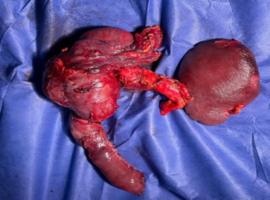
Citation: Tarif B, Oualid IS, Jbilou A, et al. Total Duodenopancreatectomy for Intraductal Papillary Mucinous Tumor (IPMT). Clin Image Case Rep J. 2025; 7(5): 567.